In an earlier post I mentioned my observations of how traumatic a trip to the emergency room can be for older people, and I promised to write about the emergence of geriatric emergency department (ED) models that provide better care for older people and can be a cost savings to the hospital.
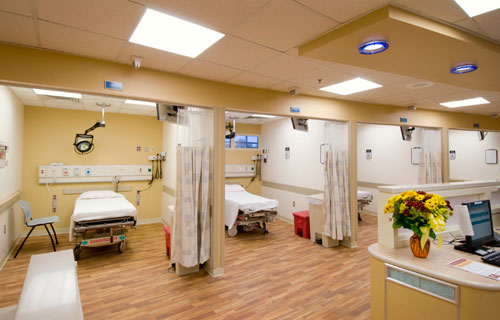 Courtesy of Holy Cross Hospital
Courtesy of Holy Cross HospitalIt seems that just as pediatric emergency units were developed to better serve children, health care professionals are recognizing that older adults need specialized emergency care, too. Their needs are different from those of younger adults.
Holy Cross Hospital in Silver Spring, MD, was the first hospital in the US to develop a new model for emergency departments that are better suited to caring for older people. The change was sparked by two things: the realization that nearly 19 percent of Holy Cross’s ED patients were 65 and older, and their CEO’s observation that Holy Cross’s ED was not well suited to care for his mother.
The basic standards for the model include fewer units, natural lighting, non-skid flooring, and soothing colors. The wall posters and pain scales have larger print, and reading glasses are available. The lighting prevents glare; the units are large enough to accommodate family member/caregivers; there are walls, not curtains and beds, not gurneys; and the mattresses are thick to accommodate the frailty of the older patient.
However, the two most important changes are related to staff training and responsibilities. A pharmacist reviews all medications of each older patient and analyzes them for possible contributions to the current medical emergency. Additionally, all ED nurses and physicians receive special training in geriatrics, and there’s a full-time geriatric social worker dedicated to the emergency room.
The geriatric social worker plays a key role in helping older adults get the care they need after discharge. I should know; my very first job as a geriatric social worker was in the emergency room of a county hospital in New Jersey. My job was to chase after families who “dumped” an older relative in the ED waiting room, hoping that he or she would be admitted to the county nursing home. If I could convince the family to return to the emergency room, I then conducted a psychosocial assessment and helped them obtain the resources and services they needed to care for their older relative. I also conducted follow-up phone calls and if necessary, home visits. In the Holy Cross ED model, the geriatric social worker may not need to chase families, but he or she tries to get to know each patient and work with the caregiver to figure out if there are underlying causes to the problem that brought the older adult to the hospital. The social worker will also follow up with a phone call after the patient is discharged from the ED.
The Holy Cross Hospital, part of the St. Joseph Mercy Health Systems, served as a pilot of the geriatric ED concept. Since then, eight more of St. Joseph Mercy’s hospitals have developed geriatric emergency departments. The uptake by other hospital systems has been slow. However, as hospitals attempt to reduce excessive readmissions of discharged Medicare patients in order to avoid a reduction in reimbursements, as required by the Affordable Care Act, they may view geriatric emergency departments as an important first step.
The data show that would be a step in the right direction. For example, a study showed that 40 percent of regular emergency room patients older than 65 who were not admitted returned to the EDs with their conditions worsened. Another study, cited in Modern Physician, found that in the three months following a hospital visit, 27 percent of elderly patients will either return to the ED, be admitted, or die. The same article notes that after setting up their geriatric ED, Holy Cross Hospital reduced its 30-day readmission rate from 10.9 percent to 5.2 percent. And another senior-friendly ED at St. Joseph Regional Medical Center in Paterson, NJ, reported that unscheduled returns of ED patients age 65 and older dropped from 20 percent to just over 1 percent.
Needless to say, I am in favor of the new model of geriatric emergency departments. I especially like the Holy Cross model, which requires geriatric training for nurses and doctors and has a full-time geriatric social worker on staff. This is the type of team that will provide the best health care to older people.
