
On Tuesday, I discussed the disappointing news that our efforts with our grantees and partners have not been successful in producing the academic capacity in geriatric medicine America needs. As promised, today I want to suggest a refinement to our theory of change and make a proposal for an additional tool in our box to do better in filling this workforce gap.
First, I will explain why a couple of obvious suggestions do not seem like promising directions to improve academic faculty production. Then I will explain an idea that I think needs to be added to our theory. Last, I will show a model grant project that I think might address the problem. I invite readers to download the spreadsheet and e-mail modifications back to me. Alternatively, if you think I'm on the wrong track, please say so. Anonymous comments are fine.
First off, a knee-jerk reaction to the shortage of faculty might be to suggest that we need more training positions, more fellowships. However, I don't think this is borne out by the evidence. Bragg and colleagues give a preliminary inventory of the different advanced training mechanisms in academic geriatric medicine, and the number of positions seems more than adequate for the demand. We at the Hartford Foundation are still pumping in $2.4 million annually in support of advanced trainees through the 28 CoEs. The Health Resources and Services Administration funds 12 Geriatrics Training Centers that can each support one or two advanced fellows in medicine (plus geriatric dentistry and geriatric psychiatry). The Veteran's Administration Geriatric Research Education and Clinical Centers–based special fellowship is available at 16 institutions for multi-year, post-clinical training. The Reynolds Foundation's FD-AGE program supports some advanced training as well. Institutional and individual research fellowships (e.g., National Institute of Health T-32 awards) are available, as are local private positions. I'm sure there are even more resources out there, but this is already enough. I don’t see the problem as a scarcity of money to develop talent, but rather a scarcity of talent that wants to be developed into a career in geriatrics, much less academic geriatrics.
Second, some might claim that we need to wait on a resolution to the many reimbursement problems affecting those caring for geriatric patients. Clearly, geriatricians who predominantly serve the slowest and sickest patients are at a disadvantage in a Medicare fee-for-service payment system, even with this year's new 10 percent Evaluation and Management bonus payments. However, these concerns are more relevant for practicing geriatricians. Academic geriatricians are subsidized by many other sources, including research grants, the need for training programs to maintain accreditation, and in some cases their health care systems.
 So what is the problem? As I see it, there is a complex interaction of the relatively low pay of geriatric medicine, the uncertainties of developing a career in academic medicine, and the life stage of the typical fellow in training. While there is conflicting evidence on the role of educational debt in career choice, I think that physicians at the end of Post Graduate Year 4 (PGY4) face a very difficult choice: if they went straight through college, medical school, and residency training, they would be around 30. If they have median educational debt they have either been deferring loan payments of $10,000 - $20,000 per year (and incurring more interest) or they have been making payments out of resident salaries of $40 to $60 k per year. Now that they have finished their clinical training, they can earn $120k to $170k in clinical practice, start paying their debts, and still have sufficient money to live comfortably and start a family. Or, they can continue to make fellowship salary for a few years and make hard choices between debt payment and other life expenses, all for the ultimate uncertainty of a soft money research or educational career.
So what is the problem? As I see it, there is a complex interaction of the relatively low pay of geriatric medicine, the uncertainties of developing a career in academic medicine, and the life stage of the typical fellow in training. While there is conflicting evidence on the role of educational debt in career choice, I think that physicians at the end of Post Graduate Year 4 (PGY4) face a very difficult choice: if they went straight through college, medical school, and residency training, they would be around 30. If they have median educational debt they have either been deferring loan payments of $10,000 - $20,000 per year (and incurring more interest) or they have been making payments out of resident salaries of $40 to $60 k per year. Now that they have finished their clinical training, they can earn $120k to $170k in clinical practice, start paying their debts, and still have sufficient money to live comfortably and start a family. Or, they can continue to make fellowship salary for a few years and make hard choices between debt payment and other life expenses, all for the ultimate uncertainty of a soft money research or educational career.
One idea I’ve been toying with for several years is a competitive “debt service” award targeting physicians in residency training who would commit early to go into academic geriatrics. Only changes in federal payment policy can move the dial on the lifetime earnings differential between a highly paid specialist and a geriatrician, but maybe there are people who are interested in the intellectual and emotional rewards of a career in academic geriatrics but are overwhelmed by the financial challenges of this choice, particularly in the short term. I recently learned that one of our Centers of Excellence is using an approach like this, and I hope they will share their experience with all of us.
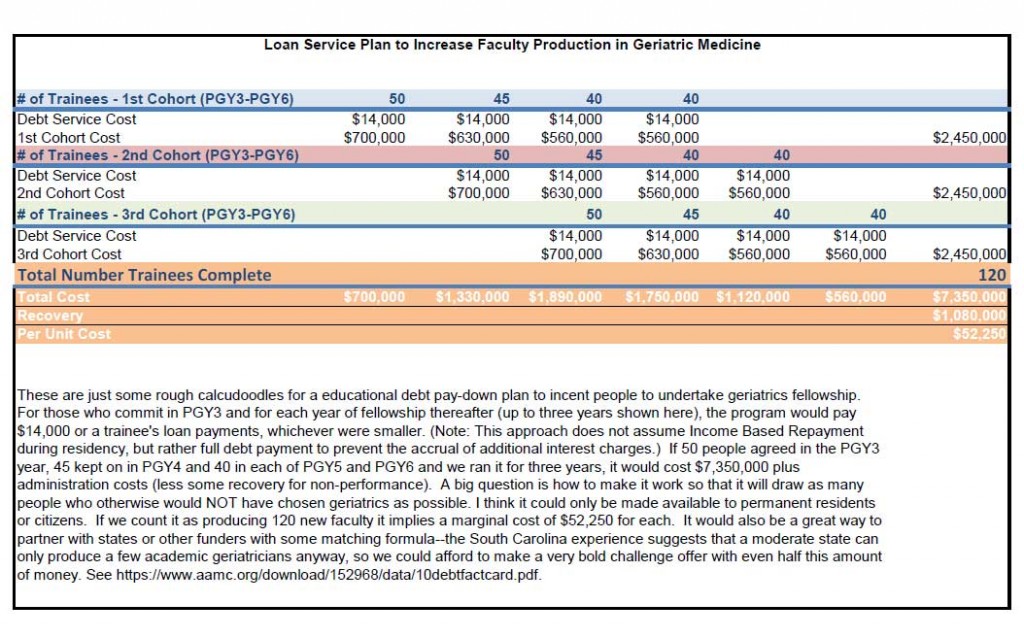
In the “debt service” approach as I imagine it, we run a competition to select residents as early as possible (PGY2) and offer to make their educational debt payments for them as long as they pursue academic geriatric training. Depending upon their debt level and interest rates, this would be around $10,000-$20,000 per year. Note we don't promise to pay off their loans, merely to make their payments for them in the particular years in which we want to influence behavior. In this approach, we take advantage of the time value of money and the relatively low income of resident physicians to influence their career choice at a critical moment. I’m not sure what markers might be used to predict success in academics at this stage of training, but given the availability of scholarly project time in residency, we could organize experiences that would quickly inform trainees and future fellowship directors/chiefs of the interests and capabilities of the awardees. Perhaps trainees who backed out early could incur minimal penalties to reduce their risks of trying, while we could impose repayment penalties for awardees who fail to follow through on their commitments after accepting more support.
Although the Foundation is not currently in a position to do this approach at a scale that would truly make a difference nationally, we might be able to start at a small scale in a year or two and by so doing create a mechanism that others could join.
Is this a reasonable idea? If so, there are many design parameters to be finalized. I invite your feedback on the approach; a generic spreadsheet with program characteristics is available here. Download it, modify it, and send it back to me. Post your adjustments as comments so others can see, and we will try to provide a “wiki-like” experience of seeing multiple proposed changes by posting links to updated spreadsheets.
If this idea doesn’t work for you, what do you see as alternatives for recruiting additional quality trainees to careers in academic geriatrics?
